
Why does cognitive load increase during perimenopause?
TL;DR: Cognitive load is metabolic load
Every decision, every emotion you manage, every commitment you track draws on the same biological resources as physical work. In perimenopause, declining estrogen reduces the brain’s buffer against this cost. The result is not weakness. It is a real physiological shift that requires support.
She sits at the kitchen table with a cup of tea, looking out the window.
Still. Present. Not frantic, not disheveled, not the stock photo version of a woman overwhelmed. Just a woman in the quiet part of the morning, before everything starts again. But look at the table around her. A child’s school paper. A laptop half-open. Her phone, face-down. The architecture of a full life, held quietly in place.
She’s not thinking about nothing. She’s running the calendar for the week while thinking about the dentist appointment she needs to reschedule, the milk that won’t last until Thursday, the work thing tomorrow, the text she promised to send before dinner, and the conversation from yesterday she’s still processing.
This is not overwhelm. This is an average Tuesday, and every bit of it costs something.
The work nobody calls work
Women don’t carry this kind of mental load because they’re unable to delegate. We carry it because this is what holding a life together looks like. The logistics, the emotional temperature, the anticipatory management of a dozen small things that would quietly fall apart without your attention.
And nobody recognizes it as work. Not because it’s not real. Because it is invisible.
Cognitive load is metabolic load
Here’s the part that changes how you think about your fatigue. Your brain does not have a category for “just thinking.” Every decision you make, every commitment you track, every emotion you manage, anticipate, or regulate draws on the same fundamental biological resources as physical work.
Intense thinking, decision-making, and emotional regulation (cognitive load) operate within the same metabolic and physiological constraints as physical exertion — consuming glucose, elevating cortisol, and triggering inflammatory pathways to manage allostatic stress.
Thinking hard triggers the same stress response and the same hormonal activation as physically training hard. The only difference is that one gets counted and one does not.

What research shows about cognitive load and cortisol
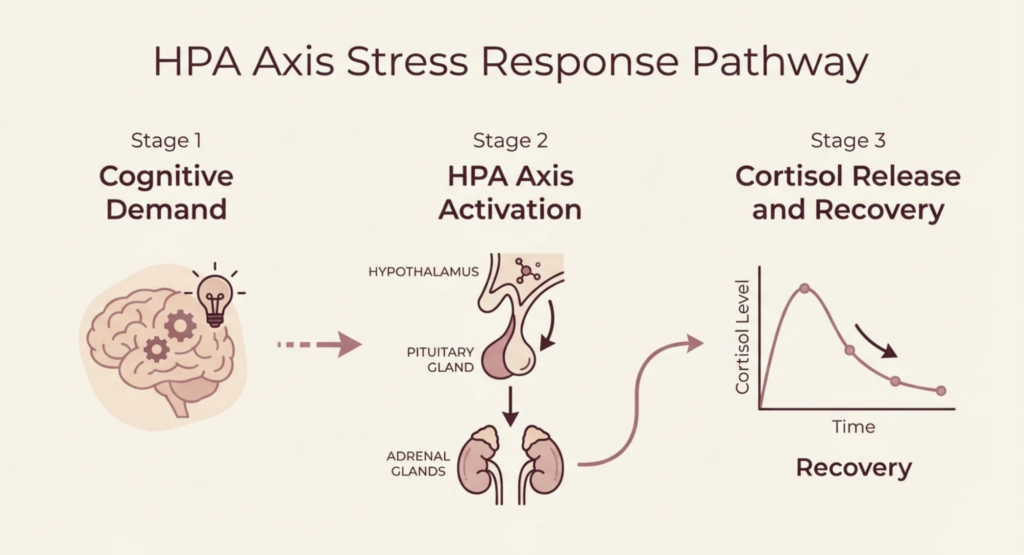
Studies on cognitive load and cortisol have consistently shown that sustained mental demand activates the HPA axis, the same stress-response pathway triggered by physical exertion. Same stress hormones. Same downstream inflammatory markers. Same pattern of nutrient depletion.
The brain consumes approximately 20% of the body’s total glucose supply at rest. Under sustained cognitive demand, that draw increases. Decision fatigue is not a productivity concept. It is a metabolic one.
The difference between cognitive labor and physical labor is not what it costs. The difference is whether anyone accounts for the recovery it requires.
Why the same cognitive load feels different at 45 than at 35
This is where perimenopause enters the picture. Not as a cause of weakness but as a shift in conditions.
Estrogen plays a significant role in the brain’s ability to manage and recover from cognitive demand. It supports glucose metabolism in the brain, reduces inflammatory signaling, and contributes to the neurological resilience that allows the HPA axis to return to baseline more efficiently after activation.
As estrogen fluctuates during perimenopause, that buffer gets smaller.
Before and during perimenopause
Before perimenopause: Estrogen is stable. The stress response is cushioned. Mental load is absorbed quietly, rarely showing the receipt.
During perimenopause: Estrogen fluctuates. The same load costs more in energy, focus, and recovery. The workload may be the same. The cost is not.
Women who carried a high cognitive load at 35 and barely registered the cost often find the same load feels genuinely different at 45. Not because they have become less capable. Because the recovery cost is higher. Because the body is now accounting for something it used to absorb without showing the receipt.
Perimenopause brain fog — the word-finding gaps, the sense of mental static, the difficulty concentrating through a long afternoon — are not signs of cognitive decline. They are signs of a brain working harder with fewer of the biological resources that used to make that work quiet. (Sandstrom et al., 2011)
The HPA axis and why recovery takes longer
When the HPA axis is activated repeatedly by high cognitive demand and the hormonal environment shifts to make recovery slower, the result is cumulative load. Each day starts from a slightly higher baseline of activation. The gap between what you carry and what the body has had time to recover from gets wider.
This is not a personal failure of resilience. This is biology, operating exactly as it should under the conditions you are actually in.
If you feel more depleted from the same life you have always handled well, there is a biological reason for that.
What would change if you recognized cognitive labor as work?
What would change if you treated your cognitive labor the way you treat physical labor?
What if, at the end of a day that contained no visible exertion but enormous invisible effort, you said: I worked hard today. And meant it. And let that name carry weight.
If you built recovery around what actually depleted you, not just what you can point to on a list.
If you stopped trying to explain your fatigue and started doing the math. The math that accounts for the full metabolic cost of running a life, not just the parts that anyone else can see.
You are not bad at rest. You have never been given credit for the work that requires it.
Naming cognitive load does not fix the problem, but it changes something
There is no version of this post that ends with five simple steps. The invisible labor does not disappear once you can see it clearly. The load does not lighten because you finally have words for it. But something does change when you stop treating your fatigue as a character flaw and start treating it as accurate feedback from a body that has been doing real, metabolically costly work for a very long time.
You stop asking what is wrong with you, and begin asking what the work actually requires. Then you support your recovery accordingly.

Can Creavitalis creatine help cognitive load during perimenopause?
As a woman in perimenopause, I created Stronger around this specific biology. Creavitalis creatine at the clinical 5g dose replenishes ATP in the brain, the cellular energy depleted by sustained cognitive demand. Rhodiola Rosea supports HPA axis recovery, reducing cortisol reactivity after cognitive and emotional stress.
Save 20% on ThriveOn Stronger when you use this special link. The discount will be applied automatically during checkout.
The original version of this article was first published here on February 20, 2026.

For ThriveOn cofounders, marriage is stronger than ever
By Amy Cuevas Schroeder
I’ve heard part of this story before because it happened to me and many other women in my age group. You hit midlife and everything seemingly goes to sh## — insomnia, pains that seemingly come out of nowhere, lack of energy.
But the story I haven’t heard is about a married couple cofounding a wellness company to help women in perimenopause. That is, until I met Victoria and Andrew O’Hare.



